HIPAA-Compliant Healthcare Tools Built Into Salesforce
cmHealth brings eligibility verification, patient intake, secure messaging, prior authorization, and payment processing into one HIPAA-compliant Salesforce experience. Healthcare teams reduce claim denials, speed up intake, and keep patient communications protected without managing separate vendor portals.


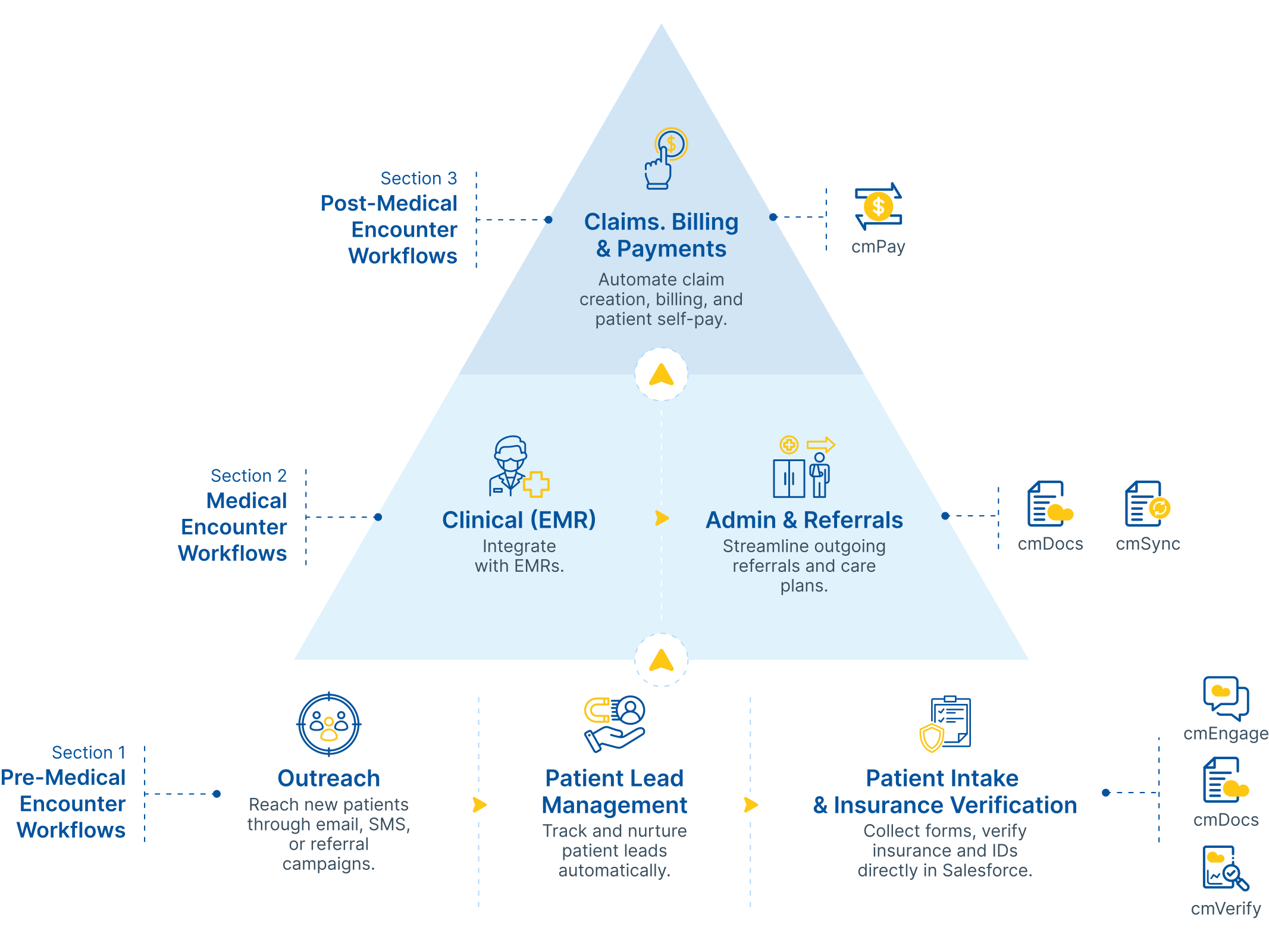
Where cmHealth Reduces Denials, Approvals Time, and Care Gaps
Faster Approvals and Payments
Real-time eligibility checks, automated authorizations, and integrated payments shorten claims cycles and improve cash flow across every line of service. Medical Insurance Verification supports connectivity with 900+ payers, helping providers verify coverage faster and reduce manual insurance validation delays.
Fewer Denials and Errors
Upfront verification and accurate data capture reduce eligibility-related denials, prevent day-of-service surprises, and eliminate costly rework. Automated insurance checks and centralized documentation help staff catch missing or incorrect information before claims are submitted.
One Connected Patient Journey
Eligibility, intake, communication, documents, and billing all run inside Salesforce, removing silos and creating a smoother experience for both patients and staff. Teams can manage patient intake, insurance verification, secure communication, and payment collection from one connected platform.
The Apps That Power cmHealth
Medical Insurance Verification
Automate medical insurance eligibility and verification with 900+ payers in Salesforce. Replace manual payer portal logins, phone-based eligibility checks, and repetitive data entry with real-time insurance verification directly inside patient workflows.
Document Generation & Signature
Generate, merge, split, digitally sign, and vault documents securely. Automate patient intake forms, consent packets, treatment agreements, disclosures, and authorization documents directly from Salesforce records.
SMS & Fax Hub
Automate and manage SMS, MMS, and fax communication. Healthcare providers can send appointment reminders, intake instructions, prescription updates, and secure patient notifications from Salesforce while maintaining communication history and delivery tracking in one system.
Payment Connect
Robust payment solution to manage credit/debit cards, and ACH payments on Salesforce. Collect co-pays, outstanding balances, recurring payment plans, and patient invoices directly within Salesforce while improving billing visibility and reducing reliance on disconnected payment tools.
Why Healthcare Teams Choose cmHealth for HIPAA-Safe Patient Workflows
Faster Claims Processing
Automated eligibility checks and streamlined intake reduce delays and keep claims moving without manual effort. Healthcare teams can verify insurance coverage, validate patient eligibility, and confirm authorization requirements before appointments to reduce claim rejections and billing delays.
HIPAA-Safe Communication
Encrypted email, SMS, fax, and eSign keep every patient interaction secure and fully compliant. Providers can securely send telehealth instructions, referral documents, intake packets, prescriptions, and patient notifications directly from Salesforce while maintaining audit-ready communication records.
Higher Data Accuracy
Real-time verification and integrated workflows prevent errors, missing details, and costly rework. Patient demographics, insurance details, authorization data, and signed forms stay connected across workflows to reduce duplicate entry and incomplete records.
Better Patient Engagement
Connected communication channels improve clarity, reduce no-shows, and enhance the patient experience throughout care. Automated appointment reminders, secure SMS updates, intake notifications, and payment communications help patients stay informed before and after visits.
Smoother Intake Workflows
Coverage checks, forms, and authorizations run together in Salesforce, eliminating fragmented tools and extra steps. Staff can manage patient onboarding, insurance verification, consent forms, and document collection from one connected healthcare workflow.
Reduced Staff Workload
Automation removes repetitive verification and intake tasks, freeing staff to focus on patient needs. Front-desk and billing teams spend less time on manual insurance lookups, patient follow-ups, and document collection during appointment scheduling and onboarding.

Frequently Asked Questions
How can I verify patient eligibility and benefits directly inside Salesforce?
Many healthcare teams connect Salesforce to real-time eligibility services so staff can confirm active coverage, benefits, copays, and referral requirements without jumping between portals. This reduces day-of-service surprises and helps prevent eligibility-related claim denials.
Can Salesforce help reduce insurance denials caused by incorrect coverage information?
Yes. When eligibility and benefits checks run before appointments, staff catch inactive plans, missing referrals, or outdated patient data early. This leads to fewer denials, less rework, and faster approvals from payers.
What does real-time medical insurance verification look like in Salesforce?
It typically works like this:
- Patient or member data is sent automatically to the payer
- Coverage details return within seconds
- Copays, deductibles, and limitations appear on the Salesforce record
- Everything is logged for compliance
This keeps intake and billing workflows moving without manual follow-up.
How do healthcare organizations manage referrals and authorizations in Salesforce?
Many clinics and health systems use integrated document generation and e-signature tools to create referrals, capture signatures, and store authorizations all within Salesforce. When eligibility and authorizations flow together, approvals happen faster and billing becomes more predictable.
Is insurance verification in Salesforce HIPAA-compliant?
It can be, as long as the system uses encrypted communication, secure messaging (email, SMS, fax), and tamper-evident records. Healthcare organizations often choose Salesforce-native tools so all eligibility checks, documents, and communications stay fully logged and HIPAA-safe.
Testimonials
Hear What 400+ Organizations Say About Cloud Maven, Inc